Who: People of all ages often come in complaining of sciatic pain; it’s the current “buzz word” that many people know. Pain down the leg(s) does not automatically mean that this is true sciatica. There are many different considerations of what it could be. Can leg pain or true sciatica be treated? Most of the time, the answer is yes.
What: Sciatica—what comes immediately to mind? Pain running down the leg? A quick Google search yields this: “pain radiating along the sciatic nerve, which runs down one or both legs from the lower back”. Is the sciatic nerve the only thing that runs down your leg and can cause leg pain? No, there are many structures that can cause leg pain other than only the sciatic nerve. The sciatic nerve is a huge nerve that starts in the low back and branches off into smaller nerves throughout each of your legs.
Where: Let’s take a closer look at specifics of true sciatica. Do you know where the sciatic nerve runs? What muscles it innervates? Can you tell and know the difference in sciatic pain versus referral pain from the low back? The sciatic nerve starts in the low back in the spinal cord from levels L4-S3 and runs down the gluteal region by the piriformis (possibly through or splitting it) down the back of the leg. True sciatica is when that nerve gets entrapped (smashed) which causes pain. Entrapments can happen in a several different locations: piriformis, long head of the biceps femoris, plus other locations after the nerve has split off and formed smaller nerves. Each of these entrapments will cause pain in different places in/on your leg. When I am referring to the “leg” I mean below the knee; if I say thigh, it means above the knee. The general term of “leg” meaning from the hip down is a big area and easily lost in translation.
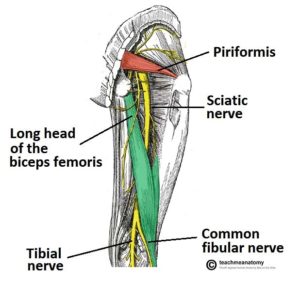
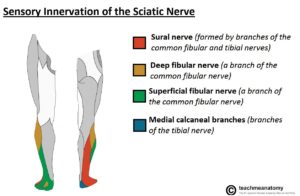
When: True sciatica will cause pain on the outside of the calf and back of the leg (not hamstring) along with the top, bottom, and outside of the foot. Many people who claim sciatica will have pain on the side of the thigh, back of the hamstrings, and possibly down into the leg and foot. These symptoms are more related to a radiculopathy which is when a spinal nerve gets entrapped/injured in your low back. These specific areas of pain often help lead us to our diagnosis.
Why: Often people ask what they did to cause this pain. It depends on what the actual cause is but many times it is due to a repetitive motion over time. I can’t count how many times someone has walked into our office with leg pain and says something like, “I don’t know what I did, it just started shooting down my leg” or “I just was trying to tie my shoe and it started”, or something similar to this.
If at times you only have low back pain, it is not sciatica. As mentioned above, sciatica will only cause pain in the leg. Other causes of low back pain could be facet joints, muscular cause, discs, or SI joints. Often times it if has been going on for a longer time and rolling/stretching doesn’t diminish it there is only a slight chance it is only a muscular cause. If rolling or stretching is going to fix it, it would have by now. In the rare and emergency case, DVT (deep vein thrombosis) typically causes calf pain and swelling. This is an emergency case that should not be ignored. As always, if you think what you are experiencing is a true emergency, call or go to the emergency department.
Other considerations: You can not see muscles, discs, or ligaments on an x-ray. The only thing that can be visually seen on an x-ray is bone and spaces between bones. Imaging is a great tool, when used in the correct context, but it is not always necessary. Often tests and functional movement screens that we perform in our office tells us what we need and how we need to treat the patient. If imaging (x-ray, MRI, etc) is needed we are able to order them.
Research shows that many people with NO low back pain, on an MRI, will have disc bulges or protrusions. Also, most MRI’s are taken laying down, this takes some of the pressure off the disc; this means that a disc bulge could possibly not show up on an MRI. That is why it is extremely important to have a knowledgeable physician do a thorough hands-on functional evaluation in office and not exclusively depend on imaging.
A wise chiropractic physician and DACBR (someone who is licensed to read imaging aka radiologist) once told me, “If you want a reason to operate on something, do an MRI”. MRI’s are the gold standard of imaging, but an MRI is only as good as the history and exam findings. Both MRI and exam findings must point to a similar diagnosis.
How can we help: At our office we see all of the symptoms listed above on a daily basis. We often look at the body in different way than other providers. Our goal is to not only reduce your pain but figure out what the problem is and teach you ways to help yourself now and in the future. The techniques and rehabilitation we use in our office focuses on the long term goal which is to help lessen the chance of the injury coming back. Our tests done in office lead us to how we are going to treat the patient and how we can help them.
We use a variety of adjusting techniques, soft tissue therapy, acupuncture, and therapeutic rehabilitation. Often our patients go home with a simple, yet specific exercise/movement to be able to improve at home. We also do in office exercises to stabilize, strengthen, and activate specific muscle groups depending on the cause. We provide hands-on care that assesses your biomechanics, minimizes risk of injury, and exceeds your healthcare goals. We educate our patients so that they understand what is going on and how they can help themselves feel better.
Here at Created For Motion, we strive to get our patients to their end goal. We want to see you succeed in your life and activities. We see all ages of patients from infants up. The office welcomes the weekend warrior to the highest athlete and everyone in-between. Are you ready to experience your best quality of life possible?
